Extent
It extends from the lateral margin of the
Location, Surface marking
It is located in the infra-clavicular region and lies along the line joining the mid point of the clavicle to the groove behind the superior pole of the coracobrachialis.
Relations
Anterior relations (Superficial to deep, Medial to lateral):
- Bone: Clavicle.
- Muscles: Pectoralis major (clavicular part) and Pectoralis minor.
- Nerves: The medial and lateral roots of the Median nerve which join to form the median nerve (brachial plexus).
Posterior relations (Superficial to deep, Medial to lateral):
- Nerves: Brachial plexus- mainly the Lower trunk, proximal part of the Medial cord, Posterior cord (+ Axillary and Radial nerves).
- Muscles: Serratus anterior (first digitation), Subscapularis, Teres major.
- Bone: Scapula
Medial relations:
- Vein: Axillary vein
- Nerves: Medial cord and its branches (Brachial plexus)
Lateral relations:
- Nerves: Lateral cord and its branches (Brachial plexus)
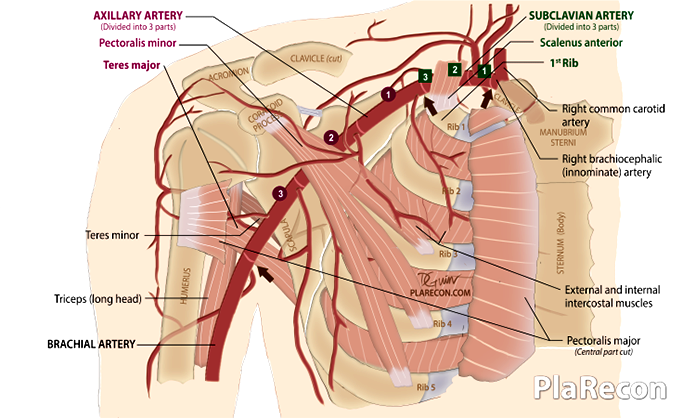
Three parts
Its divided into three parts by the pectoralis minor.
- First part: Medial/ proximal/ superior to the pectoralis minor.
- Second part: Posterior/ deep to the pectoralis minor.
- Third part: Lateral/ distal/ inferior to the pectoralis minor.
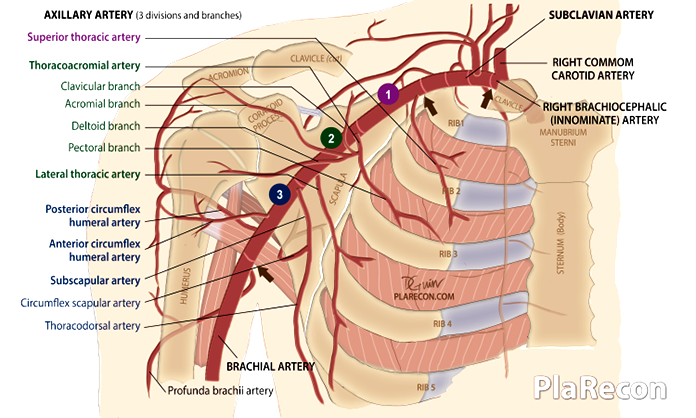
Branches
Axillary artery has six primary branches: 1 from part-1, 2 from part-2 and 3 from part-3. 💡
| First part | Second part | Third part |
|---|---|---|
| 1. Superior (highest/ supreme) thoracic artery. | 1. Thoracoacromial (Acromiothoracic) artery; branches: a) clavicular, b) acromial, c) deltoid (humeral), d) pectoral. 2. Lateral thoracic artery. | 1. Subscapular artery; branches: a) Circumflex scapular artery, b) Thoracodorsal artery. 2. Anterior circumflex humeral artery. 3. Posterior circumflex humeral artery. |
💡 MNEMONIC ➜ 1, 2-2, 3-3-3! – SALSA P.
[Color code: Axillary artery part: 1- purple, 2- green, 3- blue.]
- Superior thoracic
- Acromiothoracic (thoracoacromial)
- Lateral thoracic
- Subscapular
- Anterior circumflex humeral
- Posterior circumflex humeral
Clinical applications
1. The Basis of various Flaps
Axillary artery branches (like the femoral artery in the lower limb) form the basis of most of the conventional workhorse flaps of the thorax and back like:
- PMMC (Pectoralis major
myocutaneous ) flap–pectoral branch ofthoracoacromial artery. - LD (Latissimus dorsi) flap- Thoracodorsal artery
- Scapular and Parascapular flaps- Circumflex scapular artery
- TDAP (
Toracodorsal artery perforator) flap- Thoracodorsal artery perforator
2. Recipient vessels for free flaps
The thoracodorsal artery is used as recipient vessel for breast reconstruction using DIEP flap while other branches like the lateral thoracic artery has also been used.
The thoracoacromial trunk is used as recipient vessel for free functioning
3. Parascapular anastomosis
Branches of the three parts of the axillary artery anastomose with each other and with those of the subclavian and brachial artery around the scapula as depicted in the image below. Branches from the posterior intercostal artery arising from the subclavian artery and thoracic aorta also
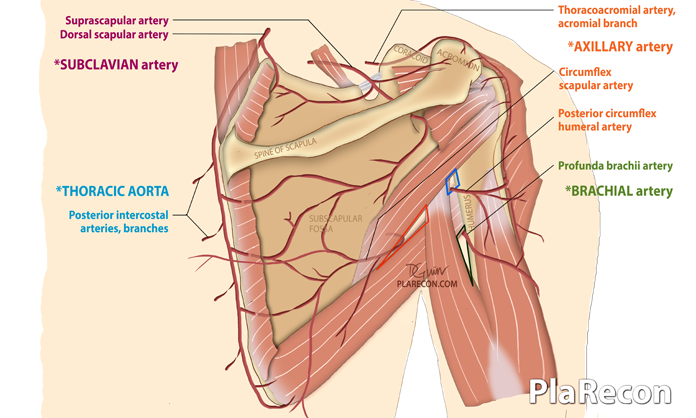
This rich system of anastomoses ensures perfusion of the upper limb in spite of injury or obstruction to a segment of the axillary artery.
Also, note the relationship of the various branches to the Triangular and Quadrangular spaces.
4. Axillary artery injury/ occlusion
Injury to the axillary artery is usually from the sharp clavicular fracture end or from penetrating trauma. Though partial injuries should always be repaired, reconstruction of segmental injuries may not be always required because of the rich anastomotic system described above. However, if there is acute critical upper limb ischaemia distally, then reconstruction has to be done using vein or synthetic graft.
Isolated axillary artery aneurysm is rare and is usually a pseudoaneurysm post trauma or crutch-induced.
Thoracic outlet compression by hypertrophy of pectoralis minor muscle, leading to axillary artery occlusion, can be seen in athletes like baseball pitchers.
5. Hyperabduction syndrome
“The second part of the axillary artery gets occluded by the overlying pectoralis minor muscle when the arm was hyperabducted and brought overhead.” This was described by Wright in 1945.
6. Axillary artery cannulation
The axillary artery is the 3rd most common site for arterial cannulation and can also be used for hemodialysis access. An associated risk is injury to closely related brachial plexus components leading to distal paresthesia/ paresis.
If you found this post useful subscribe below for more such articles & subscribe to our YouTube channel for video tutorials. You can also find us on Facebook, Twitter and Instagram.

Tutorials & tips in Plastic Surgery
+ Weekly updates of high-quality webinars!



all I have to say is THANK YOU THANK YOU
Welcome!